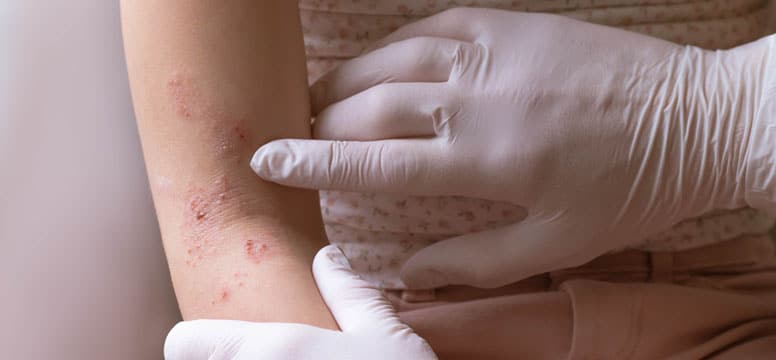
Eczema is the name for a group of conditions that cause the skin to become red, itchy, and inflamed. It’s common — over 31 million Americans have some form of eczema — but it’s not well understood. For those with eczema, it’s an itchy, red, dry irritation that can come and go for life.
Unfortunately, there is no cure for eczema. At Rendon Center, our board-certified dermatologists help patients manage their eczema.
What is eczema?
Typically, eczema causes a person’s skin to become itchy, red, and red. In extreme outbreaks, the skin can become leathery and develop cracks. Despite its prevalence, the causes of the different forms of eczema aren’t fully understood, and there is no cure. Eczema is common in infants, but it usually resolves before adulthood. For adults, it can be a chronic condition that can appear on any part of the body. There are a number of different forms, with atopic dermatitis being the most common.
What causes eczema?
Although eczema affects about one in 10 Americans, its causes are not fully understood. Normal, healthy skin works to retain moisture. This provides protection from bacteria, irritants, and allergens. In people with eczema, it appears there is a gene variation that affects the skin’s ability to retain moisture. Without the moisture, it is open to irritation due to environmental factors and allergens. Eczema seems to run in families, adding some weight to this genetic possibility.
Beyond the genetic possibilities, some scientists believe those with eczema have a skin defect that allows moisture to leave through the skin, opening the door for germs to make their way in. An overactive immune system is thought to also play a role in eczema, as it does with allergies.
Regardless of how the process occurs, when an irritant or an allergen causes the immune system to react, this produces the skin inflammation common to all forms of eczema.
What are common symptoms of eczema?
Atopic dermatitis is the most common form of eczema, so its symptoms are also the most common. These symptoms vary widely between patients:
- Dry skin
- Itching, which can be severe
- Red to brownish-grey patches that occur on the hands, feet, ankles, wrists, neck, upper chest, eyelids, inside the bend of the elbows and knees, and on the face and scalp of infants
- Thickened, cracked, scaly skin
- Raw, sensitive, swollen skin, usually from scratching
- Possibly blistering or sore formation on dry patches
Are there triggers for eczema?
Certain things can trigger flare-ups in those with the condition:
- Stress
- Contact with irritating substances such as wool, synthetic fabrics, and soaps
- Heat and sweat
- Cold, dry climates
- Dry skin
What are the different types of eczema?
There are seven different types of eczema. Unfortunate patients may have more than one type at a time.
- Atopic Dermatitis
The most common form of eczema, atopic dermatitis is chronic and inflammatory. Atopic dermatitis is related to asthma and hay fever, but it is not an allergy. Still, the immune system overreacting to irritants, whether inside or outside the body, is behind the chronic flare-ups. The symptoms listed above are for atopic dermatitis.
- Contact Dermatitis
When a person with contact dermatitis touches irritating substances or allergens, his or her skin becomes inflamed, causing it to burn, itch, and become red. Irritant contact dermatitis and allergic contact dermatitis are the most common forms. Symptoms include redness and rash, burning or swelling, and blisters that may weep or crust over. These occur on the area where contact was made.
Irritants may include these items: solvents, chemicals, detergents, paints, bleach, wool, soaps and fragrances, tobacco smoke, and allergens such as pollen.
- Dyshidrotic Eczema
This form of eczema produces small, itchy blisters on the edges of the fingers, toes, palms, and soles of the feet. Twice as prevalent in women as men, dyshidrotic eczema may be triggered by stress, allergies, moist hands and feet, or exposure to nickel in jewelry, cobalt in metal objects and some paints, or chromium salts in cement, leather, paint, and other products.
- Neurodermatitis
This form of eczema starts with an itchy patch of skin. These occur in commonly scratched areas and scratching then makes the areas more irritated and itchier. This itch-scratch cycle causes the affected skin to become thick and leathery. Neurodermatitis occurs in areas that can be reached and scratched: the head, neck, wrists, forearms, ankles, vulva, scrotum, and anus. Treatment success depends on the patient being able to resist the urge to rub or itch the affected areas, but this can be difficult as the itching can be intense.
- Nummular Dermatitis
This form of eczema looks much different than other more common forms. Patients with nummular dermatitis develop coin-shaped spots on their skin. These spots can be very itchy and difficult to treat. It is thought that nummular dermatitis can be triggered by insect bites, reactions to skin inflammation, or dry skin in the winter.
- Seborrheic Dermatitis
Another chronic form of eczema, seborrheic dermatitis appears on areas of the body where there are a lot of oil-producing sebaceous glands, such as the upper back, scalp, and the nose. This form of eczema is common in infants and is known colloquially as “cradle cap.” In adults, it also commonly appears on the scalp. Symptoms may range from dry flakes (dandruff) to yellow, greasy scales with reddened skin. It’s thought that hormones play a role in this form of the condition.
- Stasis Dermatitis
Also known as venous eczema, this occurs when the patient has a problem with blood flow in the veins and pressure develops. This pressure can cause fluid to leak out of the veins and into the skin, resulting in stasis dermatitis. This usually occurs in the lower legs. Symptoms include swelling around the ankles, redness, scaling, itching, and pain.
How is eczema treated?
First, it must be ascertained if you simply have some skin irritation or if you have a form of eczema. At Rendon Center, your dermatologist will check your skin, discuss your symptoms and your family history of eczema or allergies. That information will allow us to tell it your condition is eczema. From there, treatment options may depend on the severity of your inflammation, and what type you have.
Changing your skin care regimen is a start. It’s important to use mild soaps that don’t dry your skin. Moisturizing your skin is also important. Avoiding hot showers or hot baths is a good idea, as they can dry out your skin. Using a humidifier in the dry winter months is helpful, although that’s not as much of an issue in humid Boca Raton. Limiting stress is key.
If your eczema is more severe and stubborn, the above probably won’t be enough. We will likely prescribe these any of these possible medications:
- Hydrocortisone — These creams or ointments calm the skin inflammation.
- Antihistamines — These help calm your immune reaction.
- Corticosteroids — These anti-inflammatory drugs target serious outbreaks.
- Immune system drugs — There are several drugs, and prescription creams and ointments that control the inflammation and reduce immune system reactions. These usually can only be taken for short durations, however.
- Injectables — Dupilumab (brand name Dupixent) is an injectable medicine for severe atopic dermatitis. Typically given every two weeks as an injection, it controls the body’s inflammatory response.
- Prescription-strength moisturizers — These support the skin’s barrier against irritants and allergens.
- Ultraviolet light therapy — This can help to calm the inflammation on the skin.
- Intense pulsed light — These short duration pulses of wavelengths of high-intensity light can also calm inflammation.
When does atopic dermatitis develop and who is at risk?
Atopic dermatitis affects nearly 10 percent of infants and children, and 3 percent of adults. About 65 percent of atopic dermatitis patients are diagnosed by the time they are a year old and by age five it increases to 90 percent. The majority of patients who are afflicted with chronic atopic dermatitis will outgrow it by age 10.
The development of atopic dermatitis in many cases is genetic. When a child has a parent who has atopic dermatitis, they have a 25 percent chance of developing it, and if both parents have it, they have a 50 percent chance.
What are the symptoms of Atopic dermatitis?
Although atopic dermatitis can develop on any part of the body, it is most commonly found on the face, backs of the knees and in the folds of the arms. The rash can vary from patient to patient, but some of the common symptoms include:
- Skin that is dry and sensitive
- A persistent rash (It may go away, only to reappear)
- Intense itching sensation
- Thick scaly patches of skin
- Blisters that ooze or are crusty
Are there at-home alternative eczema treatments?
Keys to treating eczema involve knowing your triggers, bathing and moisturizing the right way with the right products, and using over the counter or prescription medication consistently. Keeping your skin moisturized can help reduce the frequency or severity of flare-ups you experience. Some changes to your daily routine that may be helpful include:
- Using a moisturizer several times a day, it helps keep your skin hydrated.
- When bathing use warm (not hot) water, do not use anything abrasive such as a washcloth.
- Always use a mild soap to help minimize irritation.
- Moisturize your skin within three minutes of concluding your shower, while your body is still moist.
There are other “alternative” treatments that could be helpful.
- Coconut oil — Studies show that coconut oil reduces the amount of staph bacteria on the skin, which reduces the chances of infection.
- Sunflower oil — Sunflower oil boosts the skin’s barrier function, helping it retain moisture.
- Cardiosperum — This extract from a tropical vine helps reduce inflammation, itching, and bacteria on the skin.
- Topical vitamin B12 — We can give you instructions on mixing this B12 compound, as there isn’t a commercial product.
- Lowering stress — Stress is a known trigger for atopic dermatitis. There are various options for lowering stress, from meditation to acupressure to massage.
Schedule Your Appointment Today!
Rendon Center can diagnose and treat various types of eczema, and many other skin conditions. Our combination of innovative technology and experience translates to superior, quality care. To schedule your visit with one of our dermatologists, contact us at 561-750-0544.

